What is hepatitis B?
Hepatitis B is a contagious virus that affects the liver. About 100,000 people in New Zealand have it. Adults who acquire hepatitis B can develop an acute illness. They may become sick soon after infection and will usually recover fully, but some can carry the virus in their blood long-term. This can lead to liver damage and liver cancer.
In these cases lifelong monitoring is needed. If you have hepatitis B, are a New Zealand citizen and are not currently enrolled with us, we invite you to register for free monitoring.
How can it be contracted?
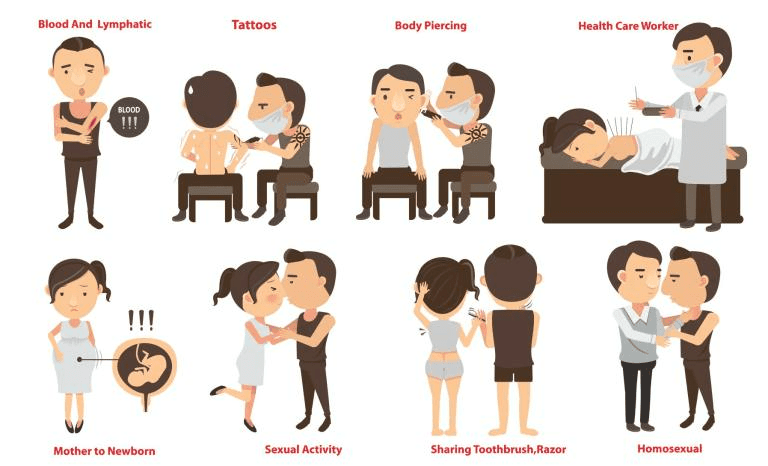
Hepatitis spreads via blood, semen and other bodily fluids. It is transmitted through:
Contact with infected bodily fluids including dried blood
Unprotected sexual contact with someone who has the virus
Injecting drugs
Receiving a tattoo using unsterile equipment
Hepatitis B can also be transmitted from mother to baby towards the end of pregnancy and during delivery. This is known as vertical transmission and is one of the most common ways people can become infected. Babies and young children who acquire the virus rarely have any symptoms. They commonly go on to have lifelong infection.
What are the symptoms?
Symptoms can include:
nausea
tiredness
dark urine
pale bowel motions
joint and muscle pain
jaundice.
Symptoms appear six weeks to six months after you catch hepatitis B.
If hepatitis B is sexually transmitted, why doesn't my partner have it?
Transmission depends on the type of sexual activity and the viral load (HBV DNA) of the infected partner.
Can I get tested and/or vaccinated?
Testing and a vaccination should be offered to the household contacts and sexual partners of people who have hepatitis B. Since 1987, all babies born in NZ have been protected against the hepatitis B virus infection through vaccination. Hepatitis B is rare in New Zealanders aged under 25.
Hepatitis B requires long-term monitoring; and six-monthly blood tests are vital.
What tests do I need?
International guidelines recommend blood tests to monitor the virus and liver are done six-monthly. These tests include:
HBsAg: Hepatitis B surface antigen
HBeAg: Hepatitis B envelope antigen
ALT: screen for active liver inflammation (and possible need for antiviral therapy)
AFP: screen for hepatocellular carcinoma (HCC). This will also be elevated during pregnancy
HBV DNA: measures the amount of virus present in the blood. May be requested every few years.
If repeated blood tests show the ALT level is up and the virus level is high, treatment may be recommended.
How can I manage the virus?
Maintaining a healthy lifestyle is important. We recommend daily exercise, avoiding fatty and sugary food and drinks, and keeping your alcohol intake to a minimum. This is one of the most important things you can do to look after your liver. Regular and heavy alcohol intake will increase liver damage, speeding up the progression of liver disease, and raise the risk of cirrhosis.
If you have cirrhosis it's recommended you don't drink at all.